If you’re looking at getting started in remote patient monitoring (RPM) today one thing becomes very obvious – it’s boring!
Think about it.
It’s full of me-too devices that are clunky and wholly uninspiring. Not to mention the patient journey lacks inspiration, is full of headaches, and doesn’t create any patient loyalty or delight.
There are no communities, no shared experiences and certainly, no one feels the iPhone-like attraction to these devices.
For an RPM program to be successful, and generate multiple six-figure revenues, you need to approach it like a startup.
But wait, what about the patient’s health, isn’t that motivating enough? No!
RPM is about asking the patient to engage in a digital health journey. You had better make it feel like an all-expenses-paid trip to Disneyland and not a one-way ticket aboard the Titanic.
This means you need to focus on the patient experience, create a compelling value proposition and grow it like an e-commerce business.
Lucky for you, we have a few tips on how you can scale your RPM program like a startup.
Table of Contents
What is Remote Patient Monitoring?
Remote patient monitoring is how physicians and hospitals can keep an eye on patients outside of the traditional clinic setting. Essentially patients are provided with FDA-approved devices that can accurately monitor a physiological signal, like blood pressure or weight.
Remote patient monitoring devices work by gathering and analyzing health data of high-risk patients and reporting that data to their doctors to determine patients’ conditions efficiently.

As long as the patient diligently monitors the physiological signal throughout a given month (16 days to be exact), the provider is able to seek reimbursement for services provided to read, analyze and interpret the data.
It can be a lucrative and low-barrier method to create additional streams of revenue for a practice that wants to expand its patient pool or services offered.
Related: Telemedicine – How It Works And How To Increase Your Income In 2024
But successfully implementing and scaling a remote patient monitoring program is easier said than done.
If you are viewing RPM as purely a bolt-on service, as 90% of folks do, it will never match the expected potential.
However, if you approach RPM as a stand-alone e-commerce business you’ll be able to attract, convert and scale a user-base that will pay multiple six-figure dividends for you.
Before we dig in, it’s helpful to understand where you fit into the RPM ecosystem. There’s no better way to do this than to follow the money.
Where Money Flows in Remote Patient Monitoring
As with most things in healthcare, there is an ecosystem to understand. RPM is no different.
Whether you are a device innovator, a health care provider or a platform service having a clear view of the RPM ecosystem is step one.
There are four main players in the RPM ecosystem:
- Providers / Hospitals
- Doctors/Qualified Health Professional
- RPM Service Providers
- Tech/device Providers
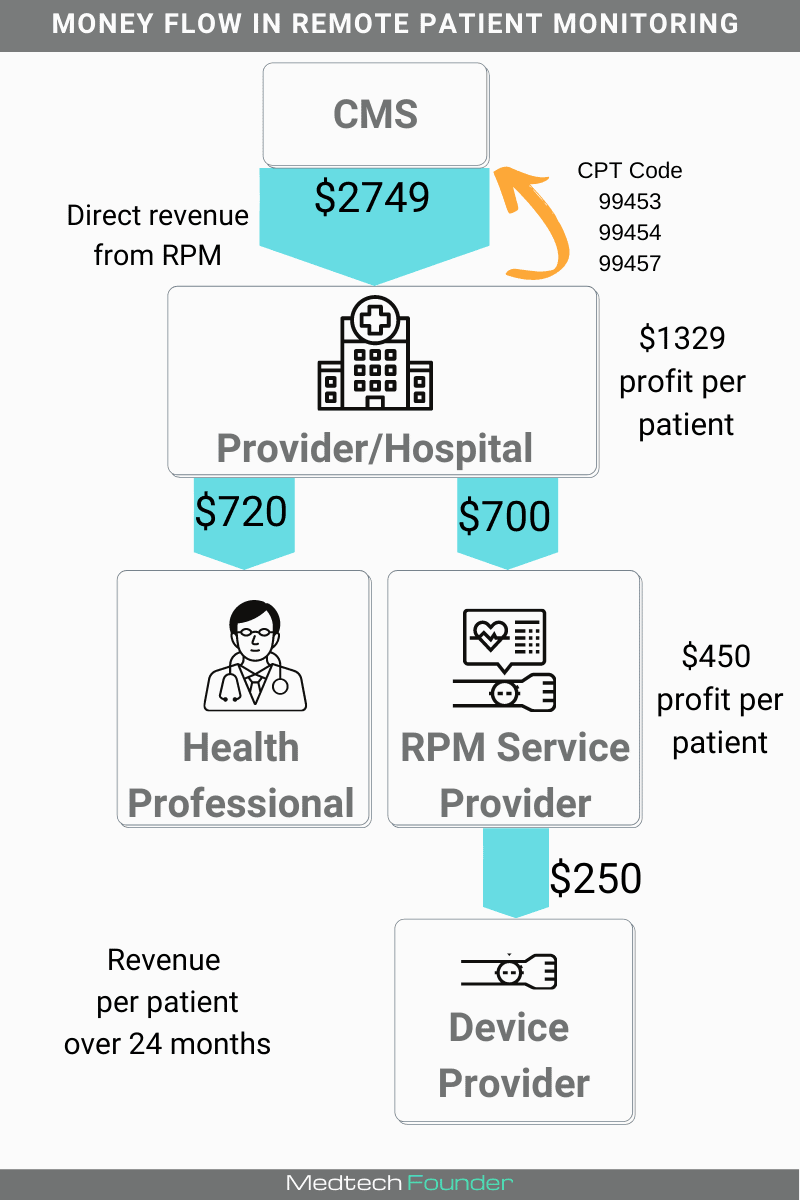
Providers / Hospitals
As a hospital, health center, or private practice you are where the patients first go to get care.
You are the “front-door”, whether digital or otherwise.
More importantly, you are the entity that is able to seek reimbursement from insurers, including the largest insurer of all, Medicare.
You have the necessary EHR systems, HIPAA compliance, and credentialed healthcare professionals to prescribe and submit reimbursement claims for RPM.
Over a two-year period, a single RPM patient could bring in $2749 in additional revenue!
Doctors and Qualified Health Professionals
You are the front lines of patient care and are making the decisions about when to use RPM with patients.
You or your staff are interfacing with patients and doing the remote check-ins and data interpretation. Ultimately your patient care and interactions lead to revenues for your employer.
RPM Service Providers
As an RPM service provider, you provide the systems and access to devices that enable doctors to practice care at a distance.
Examples include Biostrap, Athelas, 100Plus, CoachCare, Prevounce and Biofourmis.
These players integrate with existing EHR systems and provide the valuable link between devices at home and the data that doctors can monitor and review.
Every RPM provider has a slightly different pricing structure but if you assume they can bill about 25% of the hospital’s incoming RPM revenue, that’s on average $700 per patient over 2 years.
Often RPM service providers do not actually make their own medical devices. They instead contract or purchase the devices from medical device makers.
Tech/Device Providers
Finally, there are the device makers. These companies make and provide the connected medical devices that go home with patients.
RPM is based on the use of FDA-cleared devices. So device makers take on the regulatory burden of engineering medical devices and ensuring they provide accurate data.
Anything from connected scales to blood pressure cuffs are all considered a medical device if it is used in RPM.
Unfortunately, medical devices are rarely seen as exciting pieces of hardware and are mainly designed to minimize risk to the patient.
So very little energy has gone into making them exciting and rewarding for patients to use.
The companies that do this well are very rare but include players like France-based Withings.
This huge gap has been noticed by many of the leading tech companies. Companies like Apple, Samsung, Fitbit, and Google are beginning to offer FDA-cleared devices that could be used for RPM.
Their technologies are adapted from their highly successful products for the daily consumer. So usability, experience, and design are baked in.
But widespread integration of these options is not yet available.
On average a device maker can charge 20-40% of the service providers per patient revenue. That’s about $250 per device sold to RPM service providers.
What is the Reimbursement for Remote Patient Monitoring (RPM)?
Many healthcare practitioners are already familiar with video conferencing, but what does practicing medicine through the internet look like?
You are interested in broadening the scope of care that you provide to your patients remotely which will improve the quality of care you can provide.
Maybe you’re a cardiologist whose clinical practice is in Alaska – with a population density of 1.2 people/square mile and where 75% of the communities are not connected by road to a city with a hospital.
You will improve patient outcomes and improve the patient experience since they can receive care in their own home rather than coming into a clinic during the pandemic.
You want to know what technologies are available to track my patient’s sleep, blood pressure, or ECGs? How will patients learn how to use these products at home? How can I track their progress?
Start by:
- Understanding the coding and fee schedules around RPM.
- Then select an RPM provider. Several good ones offer a balance between a selection of monitoring technologies and integration with telemedicine software.
An RPM program could generate upwards of $1911 per patient annually. The exact amount depends on the patient’s locality and the specific RPM management system used.
The average range is $120-$155 a month per patient for these programs. With just 50 patients enrolled, that’s an extra $72,000-$93,000 a year of revenue potential.
Some of the leading providers of Remote Patient Monitoring devices and platforms include Withings, Biostrap, Coachcare, Prevounce, and 100Plus
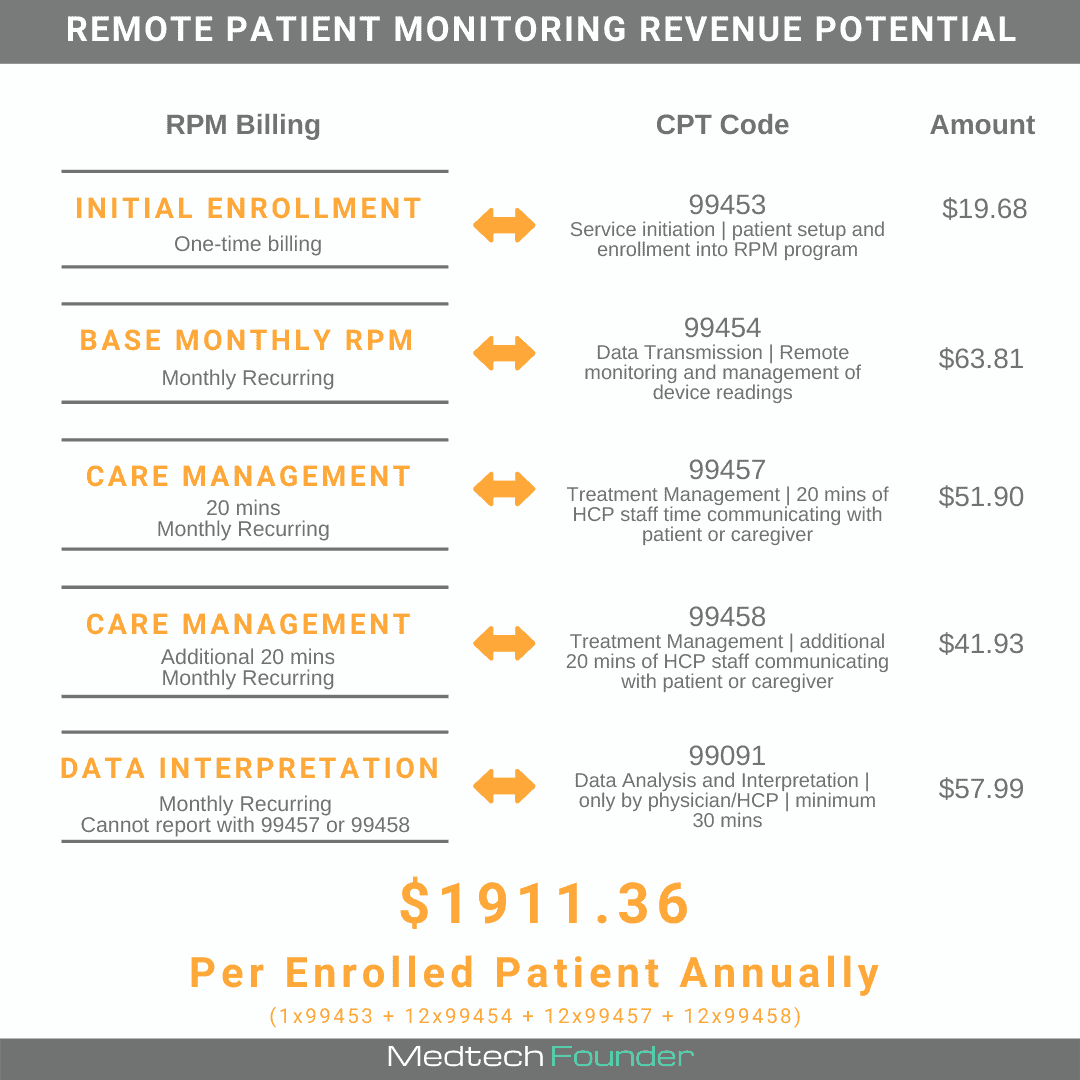
Remote Patient Monitoring Fee Schedule
Remote monitoring of physiologic parameter(s) through medical devices.
- 99453: $19.68 for initial; set-up and patient education on the use of equipment. The code requires 16 days of readings to be recorded during the 30-day billing period.
- 99454: $63.81 for initial; device(s) supply with daily recording(s) or programmed alert(s) transmission, each 30 days. Requires at least 16 days of device readings submitted by the patient within the 30-day period. Meaning, to receive reimbursement, the physician must have at least 16 days worth of readings from the patient.
- 99457: $51.90 for treatment management services, initial 20 minutes of clinical staff/physician/other qualified healthcare professional time in a calendar month requiring interactive communication with the patient/ caregiver during the month.
- 99458: $41.93 for each additional 20 minutes; frequency limitations apply.
- 99091: $57.99 for minimum 30 mins of collection and interpretation of physiologic data digitally stored and/or transmitted by the patient and/or caregiver to the physician or other qualified healthcare professional. In this instance, a QHP is qualified by education, training, licensure/regulation (when applicable). The code requires a minimum of 30 minutes of interpretation and review and is billable once in a 30-day billing period.
- Note: The data from devices used in conjunction with 99091 do not have to be from a device as defined by the FDA. There is no set number of conditions that must be monitored to meet criteria related to CPT Code 99091.
- CPT 99091 must be performed by a physician or other qualified health professional. It is not a treatment management service code but rather a data accession, review, interpretation, and modification of care plan code.
- Note that in 2020, CPT codes 99457 and 99091 could not be billed concurrently; however, in 2021, 99091 and 99457 can be billed concurrently for the same patient in the same month if all the requirements for each code are fulfilled.
- Requires no communication between patient and provider
Why RPM Sucks Today and Why Everyone is Getting it Wrong
The single biggest challenge in RPM today is engagement.
That’s why a HUGE portion of an RPM service provider’s pitch is how they address retention.
It’s also part of the reason why scaling is difficult. If the patients that you spent all this energy enrolling suddenly stop participating, you’ll never be able to create sustainable revenue
There is a very simple reason why engagement and scaling are so challenging in RPM:
You are not delighting the patient.
Let’s take a quick walk through a typical RPM patient experience.
As a patient, Instead of feeling excited that you are about to join an exclusive club of invitation-only, like-minded, and tech-advanced digital health users, most patients are at best ambivalent.
Then you receive the RPM device. You open the box and it’s clunky, usually gray in color, and feels a bit cheap. Definitely, not something that feels like it came out of the Apple Store.
Next, you go ahead and set the thing up. Great, I got a reading, now what? I guess I’ll wait until my next doctor’s check-in.
Let’s hope you remember to take the next reading. In the meantime, I’ll put this thing somewhere no one else can see it.
With this kind of user experience Is it any wonder that RPM engagement is lacking?
The solution here is straightforward.
In order to delight patients (users) you need to:
- Build a community,
- Focus on a personalized health brand
- Create a focus on intelligent health and
- Look for opportunities to use devices with the best design available.
How to Create Engagement in RPM
According to Practice Builders, almost 20 percent of patients are lost by an average medical practice annually, due to lack of service quality.
This is made worse by the fact that 7x the resources are spent converting a lead into a patient than in retaining a current patient thinking of going elsewhere.
There are many ways to create engagement. Here are some of the easiest and most effective strategies.
Build a Community
There’s a ton of ways to build community. One of the easiest and most effective ways is to create a Facebook group.
Every patient that participates in your RPM program should be encouraged to join the Facebook group. The group should be made private.
Through the group, patients can share experiences, troubleshoot, and feel like they are part of the user community. It can also be a great way to share updates, encouragement, wellness stats, and health news directly with your patients.
And importantly, there are many people using Facebook groups of all generations.
Use Personalized Health Branding
Users want to know something about the brands they use. This is a huge missed opportunity in the medical device area.
In RPM, the brand could be the RPM service provider, the device maker, or the doctor themselves.
You’ll want to think about which brand source is the strongest and create a message around the personalization that this brand enables for patient care.
Every patient wants to feel like they are being looked after. Creating a personalized health narrative related to the RPM offering is the perfect opportunity to fill this desire for the patient.
For example, say I am Doctor Smith. I would want the patient to know that Dr. Smith’s RPM program was created specifically for helping patients with hypertension. It’s uniquely suited and curated for them.
Or alternatively that Dr. Smith is using the latest digital health technology from Fancy RPM which is the fastest and most advanced provider of technology in healthcare.
As Dr. Smith’s patient, you have access to the latest and greatest.
This branding can be enforced through your practice’s or personal website. It can be enforced on a group Facebook page. Finally, it can be enforced through email reminders and traditional mail flyers (most useful for older patients).
Focus on Intelligent Health
Patients should feel as though they are part of something special and unique.
After all, not everyone is able to have access to the same kind of health insights that they will by participating in RPM.
One way to keep the concept of intelligent health front and center is to create a rewards program. Some sort of incentive for using devices well and routinely.
For example, this could include a free month (copay covered) after every 3 or 4 months of continued use. There are several loyalty software options available to get this done.
Build out an email marketing campaign about the program or post about your rewards on your social account.
And make sure your employees promote the customer loyalty program during checkout.
The more you invest in promoting your loyalty program, the more people you can turn into loyal customers.
Alternatively, you could encourage patients to set goals that could be visible to others. For example through the Facebook group.
Group-driven motivators are quite potent and help reinforce the concept of intelligently monitoring your health metrics.
Use Devices with Outstanding Design
Lastly, you should look for devices with the best design and superior build quality.
While this is often an afterthought, keep in mind that you are creating a high-engagement high-retention program.
You want patients to feel like they can show off the device. You want them to tell their friends about the cool new sensor they’re using.
For example, think of some of the most successful devices used today. Folks like Fitbit, Livongo or Dexcom come quite close to an apple-like experience for patients.
Within the world of RPM, Withings is probably one of the best in terms of design and quality for remote monitoring. Withings devices will make patients feel like they are using an upscale piece of technology.
Withings currently offers devices for sleep, weight, blood pressure, and temperature monitoring. They also have consumer-grade products like smartwatches.
If you looking for diverse activity and wellness options, Biostrap’s RPM offering is a custom digital health solution for patient care and wellness initiatives alike. Biostrap makes it simple and cost-effective with various integration options available, including the ability to white-label hardware and software offerings.
Biostrap devices (wrist, chest and arm worn) are currently being used in research in over 128 countries across the world. With clients like Pepsi Co, Regeneron and Tulane University, Biostrap offers everything you need to get started in remote monitoring.
Biostrap also supports customization through API and Bluetooth SDK integration options. Full support including custom algorithm development, streamlined access to high-fidelity raw or derived longitudinal data and all in a HIPAA-compliant research environment comes with their package.
Lastly, keep an eye on third-party consumer products from Apple, Samsung, Fitbit, Google, and others. Many of these devices are increasingly seeking FDA approval for monitoring of physiologic signals for RPM.
Having the ability to integrate data being generated from devices that patients already use will be a huge step towards engagement. In fact, making this known to patients upfront could boost your enrollment significantly.
Scale RPM like an E-commerce Business
RPM enables healthcare at home and leverages digital infrastructure. The product itself is no different than products that exist in the e-commerce realm.
So when it comes to scaling, it makes sense to use the best e-commerce strategies for RPM.
Who Does This Well Today?
There are actually a few companies that are doing this well today. Let’s look at the diabetes space.
Dexcom uses eCommerce to generate sales. In this respect, nearly 70% of all patients come across DexCom’s products for the first time through “some sort of either virtual training or online training capability or in-app capability” as per the management.
One of the fastest-growing business segments for Dexcom is e-pharmacy. The convenience and immediacy of offering the next logical product is a proven e-commerce strategy.
Creating ways to offer the obvious compliment to RPM for patients not only makes the service more valuable to them but creates more revenue possibilities for you.
Start with the Basics
Having an online landing place for patients to find you and learn all about your RPM service is a must.
Convey the benefits and success stories, have testimonials, and importantly have a way for them to sign up for eligibility.
Getting a landing page up and running from scratch can be done cheaply in just a few hours. You can get started for just $2.65/month with Bluehost. It’s the fastest way to get your project an online presence.
Use Digital Marketing
Next, consider doing some digital marketing for your RPM service. You can ease into this by taking some simple steps:
- Align with digital health-focused SEO
- Create digital assets for your service (custom imagery, photos, graphics, flyers, logos)
- Test the waters with targeted digital ads
- Create an online presence on key platforms (Facebook, Twitter, medical service platforms)
- Prioritize your lead generation options (including an email list)
- Consider creating a launch campaign
As you build your email list with contacts from your existing patient base, referrals, direct feedback efforts, personal outreach, and website, you’ll need a way to manage this efficiently.
One of the best and easiest ways to apply e-commerce best practices is to use email marketing management software.
I recommend using an email and contact list management software like ConvertKit.
This is what I use for my businesses. It is the best email marketing tool for small-to-medium audiences and is used extensively by small businesses building an audience or launching a campaign.
Scaling an e-commerce offering is a multifaceted endeavor. This can often seem overwhelming, but do not worry, there are a ton of resources to help you and the good news is that you don’t have to do it all at once or by yourself.
Just recognizing that this is a key factor to your success puts you miles ahead of most RPM programs out there today.
Here’s a full list of recommended digital marketing options for telemedicine.
How to Select the Right Launch Strategy
If you’re a practice you must first identify a need. Why should I use RPM?
It could be because your practice has high readmission rates, or you simply want to increase revenue. Whatever the reason, identifying a need for RPMs allows you to make a clear purpose for the program.
While identifying a reason why RPMs would benefit a healthcare organization is necessary, identifying a group of patients that may benefit from RPM programs is also a must.
Without eligible patients, remote monitoring is pointless, regardless of where you fall in the value chain.
Patients may be organized by chronic diseases, or whether they are high-risk or not. Practices that have an abundance of high-risk patients who need constant monitoring may benefit from remote monitoring programs.
If you’re an RPM provider, these are the kinds of practices that you want to target.
Understand that If RPM programs do not fit into existing clinical workflows, staff and patients will not adopt the program effectively.
By breaking down the phases of setting up patients for RPM programs, you can effectively understand how RPM will fit into existing workflows. These phases include:
- Defining patient eligibility for program participation
- Identifying and deploying successful marketing strategies
- Select programs with digital self-enrollment opportunities
- Integrate treatment adherence intervention programs
- Clear and effective customer support systems
How to Build for Scale
When a practice implements a remote patient monitoring program, a critical decision is whether they should lease or buy RPM devices. The budget size, practice size, and professional goals all impact what a healthcare organization may decide regarding RPM devices.
Some practices may consider initially leasing out the devices as there are lower upfront costs. However, as RPMs are shown to have high ROIs, those practices may consider purchasing their own devices. Additionally, purchasing RPM devices have a cheaper overall cost and avoid long-term contracts associated with leasing.
If you are an RPM provider, keep in mind these kinds of purchase decisions and offer your customers something that fits their needs.
The next step is identifying and enrolling eligible patients. It may be daunting to roll out RPM to every eligible patient.
Instead, it may be best to test the program out on a small group of patients. You’ll be able to evaluate the results and adjust the process. Once the process is perfected, then scaling the program to a larger population is next.
Segmenting Patients for Eligibility
To identify eligible patients, it is suggested that the entire patient population be broken down into segments.
There are various demographics to consider when evaluating patient eligibility. Start with segmenting patients by Medicare enrollment. Medicare Part B covers 80% of nationwide RPM costs. Patients are more likely to enroll in RPM programs if all or a majority of a patient’s copay is covered.
Next, patients should be broken down into short-term or long-term care segments. Long-term care usually covers patients who have chronic conditions that may last years or the entirety of a patient’s life. Short-term care may include post-surgery patients, rehab services, and wound care.
While both groups may be eligible for RPM programs, organizations may have separate portals for either group.
Once the length of care is determined, patients can then be divided by conditions and diseases. The reason patients may be separated by conditions is that patients with different conditions typically have different goals.
Recruiting
Once eligible patients are identified, the next step is recruiting those patients. There are three options that most healthcare organizations use in recruiting patients:
- In-person
- Out-reach campaigns
- Digital marketing
- Phone calls
Introducing the program to patients in person during in-office visits leads to the highest rate of success. Physicians can explain the benefits of remote monitoring and answer any questions that the patient might have.
Out-reach campaigns are an indirect way to engage possible participants. It is usually done by sending a letter to a list of eligible patients, describing what the program is, why it is valuable, and inviting them to participate.
Digital marketing lets you get in front of patients where they are – online. By conveying information about your practice, your technology, and the care they’ll receive you’ll be able to extend your reach,
It is vital to have a dedicated phone line for the RPM program that a care manager may contact eligible and enrolled patients through and for the patients to call for customer support.
Digital marketing, phone calls, and outreach campaigns can be a precursor for in-person visits. This is called setting up a Funnel.
Training
Both patients and clinicians must be adequately prepared to use remote monitoring programs. Most solutions require extensive engagement from patients, so they must understand how to use mobile apps, portals, and wearable devices.

When it comes to training patients, expectations and goals should be set ahead of time. Clinicians must also be able to answer any questions that may arise.
When training clinicians, they should focus on device utilization. It is critical that the clinician understands how to use the devices and is educated about the program because they are responsible for teaching the patients.
Additionally, patients should be able to understand levels of readings to know whether their blood pressure, heart rate, etc. is reasonable, fair, or bad. They should also know the proper steps to take based on those readings.
Leverage the Right Tools
Depending on which system you choose, the possible equipment available differs. This is important to consider when choosing or developing a system.
Some vendors may require that you use their remote patient monitoring equipment for patients in the RPM system. Other systems may be integrated with devices made by third-party manufacturers.
RPM Providers
There are various companies that utilize RPM for their brands. Fitbit, a well-known brand that offers fitness trackers and smartwatches that have found uses in healthcare industries. In 2019, Fitbit released a data-driven personal health subscription service to generate reports patients can share with their physicians. Additionally, several Fitbit devices feature third-party software support that open the gates for health data monitoring.
Biofourmis provides predictive and personalized care by utilizing active and passive data collected from clinical-grade wearable devices. These wearable devices provide continuous monitoring of over twenty physiological parameters.
Biofourmis primarily focuses on cardiometabolic disorders, pain, and oncology. Pharmaceutical companies often use Biofourmis’ RPM and AI-based analytics for digital clinical trials and as a companion therapeutic.
Sony also has a remote patient monitoring platform for healthcare providers, mobile health tech providers, health plans, and any other health service. The B2B platform provides a secure cloud system through a connected wearable device.
The company’s platform, called mSafety, constantly monitors patients on the wearable device. The device does not need to connect to a smartphone due to a built-in SIM card for constant connection.
Use Marketing Automation to Engage Patients
Marketing automation refers to allowing some of your routine marketing tasks to be handled automatically by the software.
Monitoring and keeping your patients updated manually is a time-consuming process. This is because there are so many processes to be repeated daily just to keep your practice fresh in the patient’s mind. Automation can set you at a faster pace than your competitors.
The idea is to use automation to re-engage your patients. Automation can help you communicate stronger and faster with your target audience.
Delivering excellent patient service and making it easy for patients to access vital information and support is critical. And this is one of the many reasons why you need to automate your marketing processes. For instance, Front Desk software can help you plot your patient persona, set up a marketing campaign, and collect vital patient data.
Through marketing automation, you can manage your patient contacts, send regular emails, schedule promotional newsletters and send text messages and appointment reminders. Standardizing your routine processes will enable you to deliver on the promises that you made to your patients.
Regardless of how you look at it, marketing automation can help your practice in so many ways. The most important fact is it can help you engage and retain your patients.
Execute Like a Startup
Once marketing strategies are deployed, eligible patients have been identified and contacted, and devices are secured, it is time to launch the remote monitoring program.
In the beginning, it is suggested that baseline metrics are tracked so they can be compared later in the program. Initial metrics will make it easier to identify success rates and areas for improvement.
If you planned correctly, you can have RPM up and running in as little as 2-weeks. But you must be ready to troubleshoot any technical issues and assist patients.
The manager of the RPM program should monitor incoming data to ensure that everything is working smoothly and as intended. Patients who are not taking readings as often as they should need to be contacted or reminded to promote active device usage.
As the program continues, you can adjust based on patient and staff feedback.
Success largely depends on how effectively patients and staff are trained on remote patient monitoring.
To ensure that patients and staff are well educated on the program, you should consider reviewing the following factors with the staff on the ground:
- Define remote patient monitoring
- Describe how it works
- Explain the value of remote patient monitoring
- Provide instructions on device setup and usage
- Deliver RPM education through multiple channels
- Strengthen RPM education
Bottom Line
Executing a remote patient monitoring program successfully requires careful research and planning. RPM use will continue to rise but only practitioners who approach it like a stand-alone digital business will see consistently high ROIs
The advantages of RPM far outweigh any disadvantages for both the business and the patient. Home health monitoring and mobile health services allow providers to continuously capture, monitor, and automate healthcare data analysis. Patients may completely eliminate any need to physically visit their doctors as some of these software systems allow doctors to examine and even treat patients remotely.







Join the discussion 2 Comments